Telehealth is everywhere just now.
The Government is keen, and has a delivery plan: they hope it will keep people out of hospitals and care homes (i.e. save money). Industry is keen: devices in every home, charged at healthcare prices – what’s not to like? Yet another article singing the praises prompted me to share some scepticism. Don’t get me wrong, I’m quick to experiment with new IT systems. Show me a gadget and I’ll check my bank balance to see if I can get one. But somehow the telehealth claims don’t stack up.
What is telehealth?
The Scottish Centre for Telehealth say: “The provision of health services at a distance using a range of technologies.” Other terms include telemedicine (provision of healthcare at distance by a healthcare professional), telecare (use of technology to support patients with long-term conditions in their home), and the all-embracing telehealthcare. So basically, anything to do with health or social care, and communication of information over distance. Defined this broadly, it’s hard to say it won’t work!
Some examples of telehealth
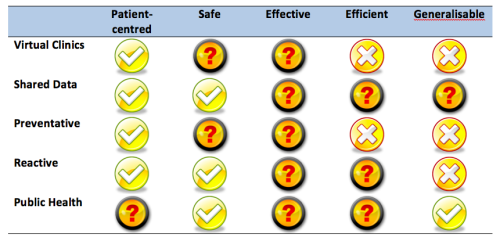
So let’s judge some specific examples against patient-centredness, safety, effectiveness, efficiency and generalisability:
- Virtual clinics Using videoconferencing to avoid travelling to see a specialist is a boon for patients living in Scotland’s remote islands (most people don’t). However, it’s only useful if the clinician doesn’t have to examine you. Anyone who uses VC also knows that subtlety of communication is not its strong point. The equipment costs are coming down, but the main cost is clinician time, and that is, at best, unchanged.
- Patient access to records RenalPatientView is an online portal available to most renal patients in the UK, which provides access to blood results, correspondence and medication lists, together with information to assist interpretation. Patients can enter their own data (eg blood pressure), and in the future, that may enter the health record. The evaluation showed it was appreciated by the subset of patients who used it. Whether it improved outcomes or was cost-effective remains moot.
- Preventative interventions Home measurements, usually with data upload for central monitoring, is being tried in various long-term conditions including COPD, heart failure and diabetes. The Whole System Demonstrator was a large randomised trial of 177 GP practices. In this high risk population (median 8-12 patients per practice), the telehealth intervention reduced mortality (by 3.7%) and reduced hospital bed days (by 0.8 days per patient) over a year. There are some doubts about the control arm of the study, and the economic analysis was not cost-effective at £92,000 per QALY, substantially above the usual threshold.
- Reactive interventions Monitoring may allow rapid intervention when things go wrong. Alert bracelets can summon help after a fall. GPS monitoring of patients with cognitive impairment may reassure patients and families. How cost-effective they are, will depend on what they prevent (hospital admissions or moving to a care home?). The effect size will be mainly determined by who they are given to. The lower the threshold for use, the less effective they become.
- Public health interventionsThere are many smartphone apps to monitor health and fitness. Currently, I’m playing with:
- Pacer, a fancy pedometer that alarms if I sit still too long. I’ve learned I don’t walk enough.
- SleepBot, monitors sleep by detecting movements in bed. It seems I don’t sleep enough, and if I drink alcohol, sleep quality deteriorates.
- MapMyWalk, tracks walks I’ve done, and their distance. I still don’t walk enough.
I have a sneaking suspicion these apps are not the answer to the obesity epidemic, but just the latest version of Jane Fonda’s workout video, or that David LLoyd gym membership.
The personal touch
So here’s my basic issue. I can book my holidays online, and I don’t miss the travel agent (though it does seem to take me longer). I can bank online, and I don’t miss the bank clerk (except when things go wrong). But healthcare is about individual relationships between patients and healthcare professionals. Most healthcare is one to one, or a many to one relationship. Most healthcare expenditure is on staff. So to reduce costs, telehealth will have to reduce the amount of time spent by healthcare staff on individual patients, without reducing the quality of care. Can that circle be squared?
Oh! Look at the shiny box…
I realise this blog is a hostage to fortune that I’m going to have to explain away in 10 years time, but… I accept telehealth improves patient experience. I remain dubious that it improves health outcomes, except in highly selected groups. I don’t believe it can save money to any great extent. The Medical-Industrial Complex promoting telehealth is a dangerous combination of governments thinking they will save money, and industries thinking they will make money. Like any other intervention, telehealth needs evidence to show effectiveness, safety and cost-effectiveness. So Telehealth Advocates, prove me wrong…
This week’s blog, leading off a month of blogs by medics, was by @micmac650 (Mark Macgregor), who is an Associate Medical Director in NHS Ayrshire & Arran.
Courtesy of Mark Macgregor at Ayrshire Health
Comments
No responses to “Telehealth: So obvious, it must be true”